Glaucoma Treatments
-
Content written by Annie Tye, Ph.D | Reviewed by Joseph Christenbury, M.D. | Last updated 10/20/2023
- Overview
Overview
What is glaucoma?
Glaucoma is a group of eye diseases where the optic nerve has been damaged by high pressure within the eye. It is one of the leading causes of blindness in people 60 or older. While it is more common in older adults, it can occur at any age.
What are the causes?
Glaucoma is caused by elevated eye pressure, or intraocular pressure (IOP), due to fluid buildup in the eye. Normally, this fluid drains through a specialized tissue, called the trabecular meshwork, at the angle where the cornea and iris meet. Sometimes, this drainage system is blocked, or your eye makes too much fluid, which increases IOP. As this pressure continues to build, the optic nerve may be damaged, leading to vision loss in that eye.
Cost of glaucoma treatments
The cost of glaucoma treatments can vary widely. Here are some average costs for various types of treatment options:
- Medications:
- Eye drops: Generic eye drops cost around $10 to $50 per month, while brand-name drops can be more expensive.
- Oral medications: $25 and $100 per month.
- Laser Therapy:
- Laser trabeculoplasty: $1,000 to $2,000 per eye.
- Laser iridotomy: $1,000 to $2,000 per eye.
- Surgical Procedures:
- Trabeculectomy: $2,000 and $5,000 per eye.
- Glaucoma drainage devices: $3,000 and $6,000 or more per eye.
- Ongoing Monitoring:
- Regular eye examinations may cost between $100 and $200 or more per visit.
How is glaucoma diagnosed
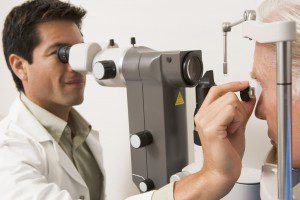
A comprehensive medical and eye examination are typically performed to diagnose glaucoma.
In order to diagnose glaucoma, your ophthalmologist will perform a comprehensive medical and eye examination. The following tests and procedures may be performed according to the Glaucoma Research Foundation:
- Detailed medical history: Your doctor will ask you about your currently medical conditions, especially if they may impact your eye health (diabetes, high blood pressure, etc.) They will also want to know the symptoms you’re experiencing, and if anyone in your family has a history of glaucoma.
- Tonometry: This exam is used to measure your IOP. With your eye numbed, your doctor will use a tonometer to gently apply pressure to the eye. Normal eye pressure ranges from 12-22 mm Hg; glaucoma is diagnosed when eye pressure exceeds 20 mm Hg.
- Ophthalmoscopy: During this procedure, your doctor uses a small device with a light to look at your optic nerve for possible damage.
- Gonioscopy: This exam is used to look at the angle where the iris meets the cornea in your eye. This is used to diagnose angle-closure glaucoma (narrow and closed angle), or open-angle glaucoma (wide and open angle).
- Perimetry: This test is used to help your doctor determine if your vision has been impacted by glaucoma by measuring your central and peripheral (side) vision.
- Pachymetry: This exam is used to measure the thickness of your cornea. People with thin corneas are at an increased risk of developing glaucoma.
Risk factors for glaucoma
Glaucoma can occur in anyone, but there are risk factors that increase your chances of developing it. These can include:
- Increased age (60 years or older)
- Diabetes
- High blood pressure
- Long-term steroid use, such as corticosteroid eye drops
- Being extremely farsighted or nearsighted
- Previous eye injuries or surgeries
Familial risk factors also contribute to your chances of developing glaucoma. If a member of your family has had glaucoma, your chances of developing it increase. If you are of Black, Asian, or Hispanic descent, your chances also increase.
Types of glaucoma
There are two main types of glaucoma that can develop: open-angle (chronic) glaucoma, and angle-closure (acute) glaucoma. In addition, there are variations of glaucoma that can develop.
Open-Angle (Chronic) Glaucoma
Open-angle glaucoma is the most commonly diagnosed form. In this type, the trabecular meshwork is partially blocked, preventing fluid from draining out of the eye. This causes pressure to gradually build up, damaging the optic nerve. Symptoms include:
- Blind spots in your peripheral or central vision; may be in one or both eyes
- Tunnel vision that develops in advanced stages
Angle-Closure (Acute) Glaucoma
Angle-closure glaucoma, also known as closed-angle glaucoma, forms when the iris bulges forward and blocks the drainage angle between the cornea and iris. Fluid will not circulate through the eye properly, and the pressure increases. In some cases, a patient may have a narrow drainage angle, making them more susceptible to angle-closure glaucoma. Symptoms include:
- Eye pain and redness
- Nausea and/or vomiting
- Severe headache
- Blurred vision
- Halos forming around lights
Normal Tension Glaucoma
Normal tension glaucoma (also known as low-tension or normal-pressure glaucoma) occurs when there is damage to the optic nerve with no increase in IOP. Your risk of developing normal tension glaucoma increases if you have a family history of the condition, are of Japanese ancestry, or have a history of systemic heart disease. The exact causes are still unknown.
Congenital Glaucoma
Congenital glaucoma develops in infants and children and is caused by defects in the eye’s drainage system. These defects lead to fluid buildup and increased IOP, which damages the optic nerve. This is a rare condition that can be passed down through family and is usually treated through surgery and medication.
Secondary Glaucoma
Secondary glaucoma often occurs as a side effect of eye injury, inflammation, advanced cases of diabetes or cataracts, or use of steroids. In rare cases, it can develop after eye surgery. Treatments for secondary glaucoma can vary depending on the underlying cause, but usually include a combination of surgery and medication.
Glaucoma treatments
If you are diagnosed with a form of glaucoma, it is important to receive immediate treatment to prevent any more damage from occurring to the optic nerve. Signs and symptoms will vary depending on the type and stage of the condition.
Unfortunately, there are no treatments available to cure glaucoma. Instead, your doctor will focus on stabilizing your eye pressure to prevent further damage to vision.
Laser-Based and Surgical Treatments
- Laser trabeculoplasty: This procedure treats open-angle glaucoma and can typically be performed in your eye doctor’s office.
- Filtering surgeries: An incision is made in the sclera (the white of your eye) and remove part of the trabecular meshwork in a trabeculectomy or make small incisions in a trabeculotomy.
- Drainage tubes: Implant drainage tubes to drain excess fluid.
- Minimally invasive glaucoma surgery (MIGS): Umbrella term for procedures that can lower your intraocular pressure without high risks as trabeculoplasty or drainage tubes.
- Laser peripheral iridotomy: Small incision in your iris to drain aqueous humor from eye. Used primarily for medical emergencies with angle-closure glaucoma.
Medications
Medications are also used to help control and reduce IOP. Eye drops are used daily to control eye pressure. These contain a number of drugs that work to limit fluid production, or help it drain from the eye better. Oral medications are also available if eye drops are not effective enough alone. This is typically a carbonic anhydrase inhibitor that works by limiting fluid production in the eye.
Can glaucoma be prevented?
Unfortunately, there’s no cure for glaucoma, but early treatment can often stop the damage and protect your vision. Be sure to visit your eye doctor annually for your preventive eye exam. Routine tests performed during these exams may identify optic nerve damage and other eye issues before they become more serious. The earlier glaucoma is recognized, the earlier treatment can begin.
EnhanceMyself.com relies on sources such as professional medical organizations, government agencies, academic institutions, and peer-reviewed scientific journals to write it’s articles. Learn more about how we ensure our content is accurate, in-depth, and unbiased by reading our editorial guidelines.
*Medical Disclaimer: This website does not provide medical advice. Read more.

